Introduction
Nephrotic syndrome is a group of symptoms that occur when the kidneys are not able to properly filter waste products from the blood. Nephrotic syndrome is defined as the presence of:
- Proteinuria
- Hypoalbuminaemia
- Peripheral oedema
It is important to note that the term nephrotic syndrome refers to a presentation of disease rather than being a disease itself. It is generally associated with the development of glomerulonephritis.
Glomerular diseases can present with features of both nephrotic and nephritic syndrome; both syndromes are considered as part of a spectrum, with some diseases being more likely to present with features of one of the syndromes.
Causes
The cause of nephrotic syndrome can vary and can be classified into primary and secondary causes. Primary nephrotic syndrome is caused by a malfunction in the kidney itself, while secondary nephrotic syndrome is caused by an underlying condition such as diabetes mellitus or amyloidosis.
Primary renal disease
Conditions usually presenting with nephrotic syndrome features include:
- Minimal change disease
- Focal segmental glomerulosclerosis (most common cause in adults)
- Membranous glomerulonephritis
- Thin basement membrane nephropathy
Conditions presenting with mixed nephrotic and nephritic syndrome features include:
- IgA nephropathy
- Membranoproliferative glomerulonephritis
Secondary renal disease
- Diabetic nephropathy
- Sarcoidosis
- Autoimmune: Systemic lupus erythematosus, Sjogren’s syndrome
- Infection: Syphilis, hepatitis B, HIV
- Amyloidosis
- Multiple myeloma
- Malignancy
- Vasculitis
- Drugs e.g. gold, penicillamine, captopril, NSAIDs
Pathophysiology
Glomerular disease allows proteins to be filtered and excreted in urine, which also leads to hypoalbuminaemia. Consequently, peripheral oedema develops because of the loss of serum oncotic pressure as illustrated by Starling force’s law equation.
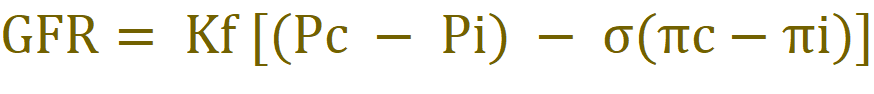
Pc: Capillary hydrostatic pressure
Pi: Bowman’s capsule hydrostatic pressure
σ: Reflection coefficient
πc: Capillary oncotic pressure
πi: Bowman’s capsule hydrostatic pressure
Clinical features
Clinical features of nephrotic syndrome include:
- Frothy urine: due to hyperlipidaemia and fatty casts in urine
- ↑ Risk of thromboembolism: due to loss of antithrombin III in urine
- ↑ Risk of infection: due to loss of IgG and tissue oedema, which compromises the local blood supply and immune response)
- Generalised symptoms, including fatigue and reduced appetite
Investigations
Investigations are aimed at diagnosing the underlying cause and are the same tests performed when investigating glomerulonephritis, which are as follows.
Urine tests
- Urine dipstick
- Urine microscopy and culture
- Urine albumin:creatinine ratio
Blood tests
- Urea and electrolytes
- Full blood count
- C-reactive protein
- ESR
- HbA1C
- Immunology:
- Complement levels
- ANCA
- ANA
- Anti-dsDNA
- Anti-GBM
- ASOT
Imaging
- Renal ultrasound scan
- Chest x-ray
Invasive tests
Renal biopsy
Management
Treatment options for nephrotic syndrome vary depending on the underlying cause of the condition. In cases of primary nephrotic syndrome, treatment typically involves the use of corticosteroids and other immunosuppressive drugs. In cases of secondary nephrotic syndrome, treatment is directed at the underlying condition.
Complications
Complications of Nephrotic Syndrome can include an increased risk of infection, blood clots, and kidney damage. Additionally, individuals with Nephrotic Syndrome are at an increased risk of developing high blood pressure and heart disease.








0 Comments